If your neck and arms become red and itchy after only a little sun exposure, it may be difficult to dismiss it as simple heat rash. In particular, if tiny rash-like bumps or hives recur in similar areas every spring and summer, it is worth checking for what is commonly called sun allergy—that is, a photosensitive skin reaction.
Sun Allergy Causes, Symptoms, and Prevention
A Checklist for Recurrent Itchy Rashes
Sun allergy is not so much a single disease name as a broad term for several photosensitive skin conditions in which the skin reacts excessively to sunlight, ultraviolet rays, medications, cosmetics, plant-derived substances, and other triggers. Symptoms can vary, including itching, red rashes, papules, blisters, and hives, so identifying the cause and protecting against UV exposure are important.
Medically, skin reactions caused by sunlight are divided into several types, such as polymorphous light eruption, solar urticaria, photoallergic reactions, and photocontact dermatitis. Although people often call them “sun allergy,” they may actually include immune reactions, drug-induced photosensitivity, reactions between UV light and ingredients in cosmetics or perfume, and reactions that occur when plant substances combine with UVA.
Mild cases may improve simply by reducing sun exposure and soothing the skin. However, if blisters form, pain is severe, the face or area around the eyes swells, or the same symptoms recur every year, it is best to see a dermatologist to identify the exact type.
Basic Information About Sun Allergy
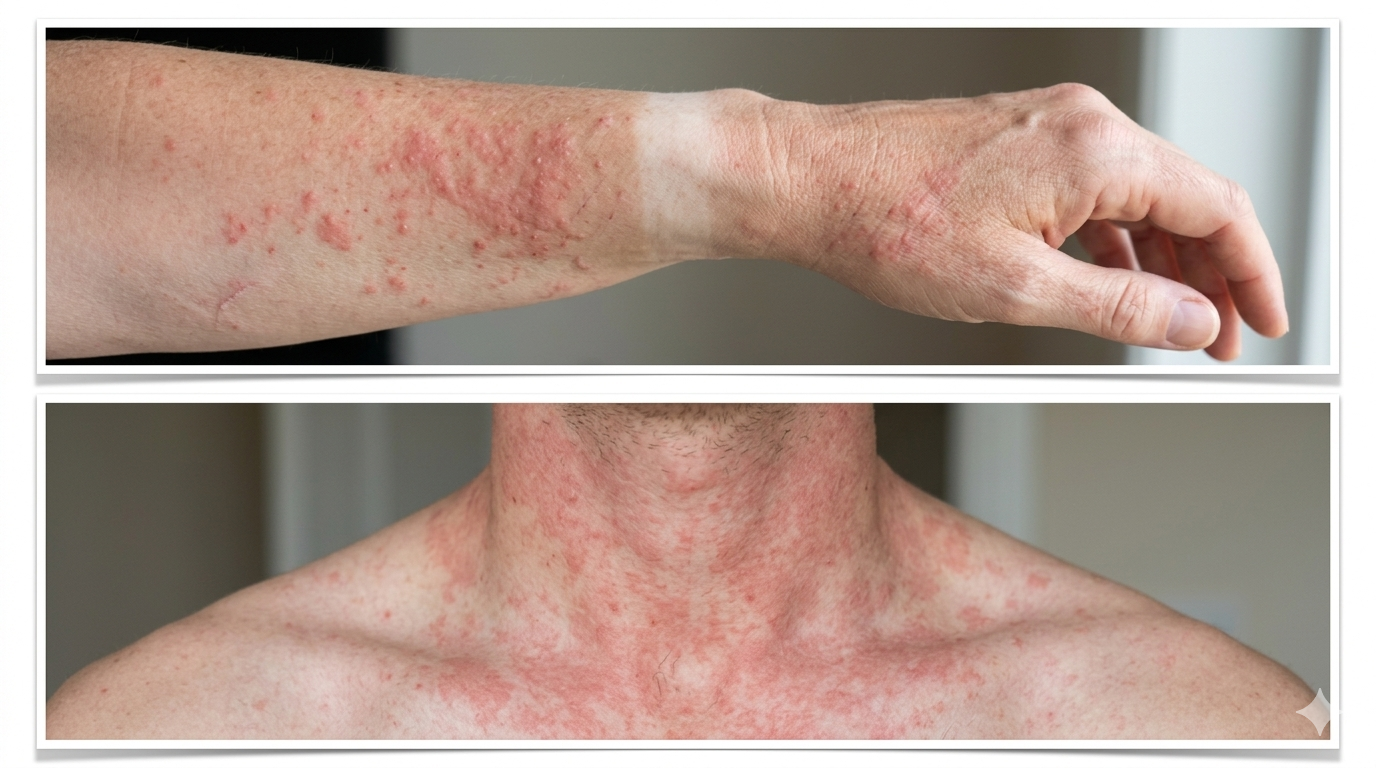
Symptoms That May Suggest Sun Allergy
Itchy red rash
Red spots or bumpy rashes may appear on newly sun-exposed areas such as the neck, upper chest, arms, and backs of the hands. Polymorphous light eruption is described as a representative type that may appear several hours to several days after sun exposure.
Tiny papules and blisters
The skin may not only become red but also develop tiny papules or small blisters. Because scratching increases the risk of secondary infection and hyperpigmentation, it is important not to scratch with your nails.
Sudden swelling like hives
Solar urticaria may cause the skin to swell like hives relatively quickly after sun exposure. If symptoms spread rapidly or are accompanied by dizziness or shortness of breath, emergency medical care is needed.
Stinging, burning, and peeling skin
Phototoxic reactions may appear as stinging and burning similar to an excessive sunburn. They can occur when medications, plant-derived substances, or perfume ingredients act together with sunlight.
How It Differs From a Simple Sunburn
| Category | Sun allergy/photosensitive reaction | Sunburn | Check point |
|---|---|---|---|
| Conditions of onset | May recur even after brief exposure | Occurs after prolonged exposure to strong sunlight | If it recurs despite short exposure, check for photosensitivity |
| Symptoms | Itching, rash, hives, papules, blisters | Redness, burning, pain, peeling | If an itchy rash is central, sun allergy is possible |
| Cause | Immune reaction, medications, cosmetics, plant substances, ultraviolet rays | Skin damage caused by UV radiation | Check whether you recently started a new medication or cosmetic |
| Recurrence | May recur every spring and summer | Occurs depending on the degree of exposure | If the same area recurs every year, medical evaluation is recommended |
Four Major Causes
1. Hypersensitivity to ultraviolet rays
This is explained as a process in which components in sun-exposed skin change and the immune system recognizes them as a stimulus. The exact cause varies by person, and in some cases it begins after the first strong sun exposure in spring.
2. Drug-induced photosensitivity
Some antibiotics, anti-inflammatory pain relievers, acne medications, diuretics, heart medications, and others can trigger light-sensitive skin reactions. If a rash develops on sun-exposed areas after starting a new medication, check the medication information and consult the prescribing clinician.
3. Ingredients in cosmetics, perfumes, and disinfectants
When perfume, essential oils, certain cosmetic ingredients, disinfectants, and similar substances are on the skin during sun exposure, photocontact dermatitis or hyperpigmentation may occur. This may be suspected especially if areas where perfume was applied, such as the neck and wrists, repeatedly react.
4. Reactions between plant substances and sunlight
If ingredients that can cause photoreactions—such as lime, lemon, celery, and some plant saps—get on the skin and are then exposed to UVA, blisters and hyperpigmentation may occur. It is important to wash your hands after outdoor cooking, camping, or handling fruit.
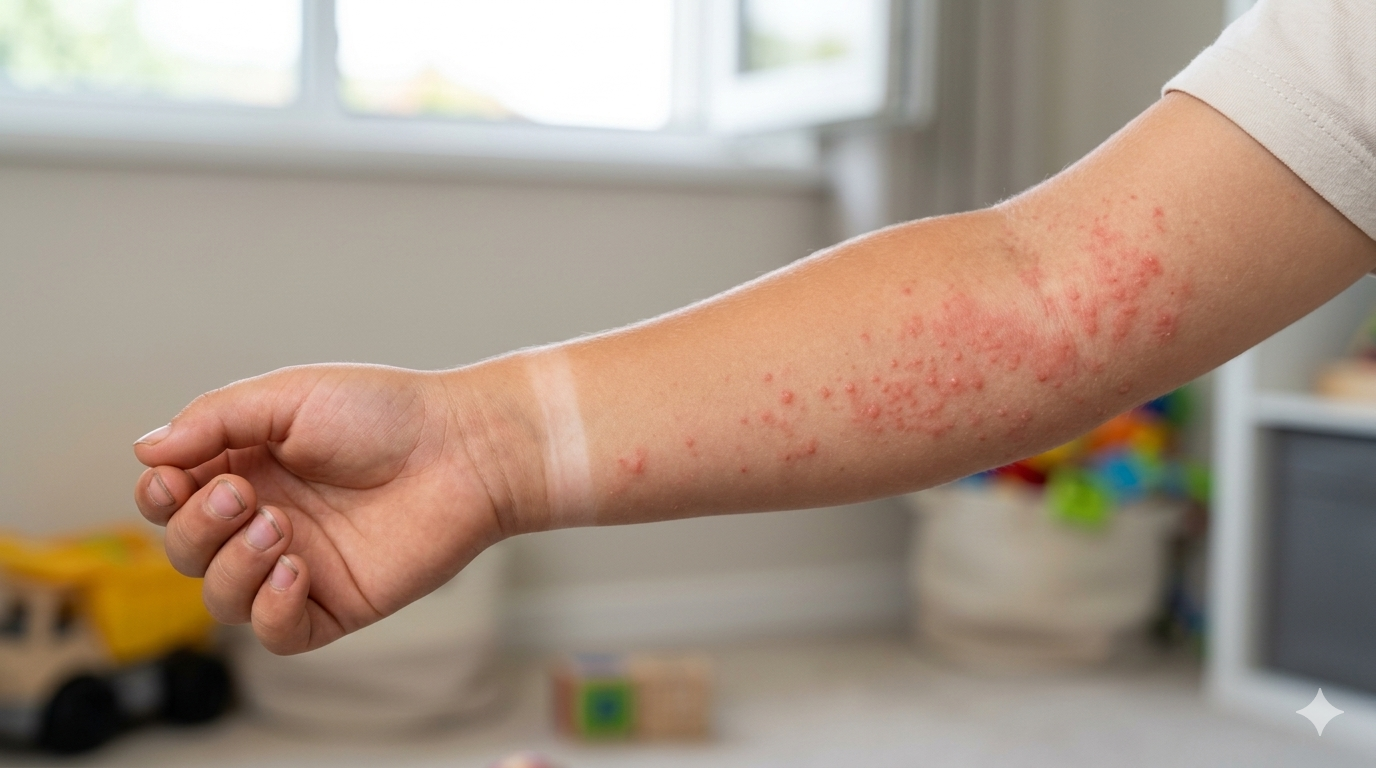
What to Do When Symptoms Appear
1. Move immediately into shade or indoors
When symptoms begin, the first step is to avoid further sunlight. If you continue outdoor activities while the rash area remains exposed, itching and redness may worsen.
2. Apply a short cold compress with a cool towel
Place a soft towel soaked in cold water on the skin to lower the skin temperature. Avoid applying ice directly to the skin because it can be irritating, and repeat short applications of about 10 minutes at a time.
3. Do not scratch; protect the skin barrier with moisturizer
Scratching because it itches further damages the skin barrier and increases the risk of hyperpigmentation or infection. Avoid strongly fragranced products, and apply a thin layer of a low-irritation moisturizer to reduce skin dryness.
4. See a dermatologist if it recurs or is severe
Mild symptoms may settle when sun exposure is avoided, but medical care is needed if there is pain, blisters, oozing, a widespread rash, or recurrence every year. Depending on the situation, antihistamines, steroid ointments, phototesting, or medication adjustment may be considered.
A UV-Protection Routine for Prevention
| Situation | What to do | Precautions |
|---|---|---|
| Before going out | Use a broad-spectrum sunscreen that blocks both UVA and UVB, SPF 30 or higher | For sensitive skin, test a small amount before applying a new product to the entire face |
| During outdoor activity | Reapply every 2 hours and after sweating or water activities | A higher SPF does not mean the reapplication interval becomes unlimited |
| 10 a.m. to 4 p.m. | Reduce prolonged exposure during hours of strong sunlight | UVA exposure can occur even on cloudy days |
| Clothing | Use wide-brimmed hats, sunglasses, parasols, and tightly woven long-sleeved clothing | Thin, loosely woven white T-shirts may provide low protection |
| In cars and by windows | Consider UVA exposure through windows as well | If driving or sitting by a window for a long time, arms and backs of the hands need protection |
When Medications or Cosmetics May Be the Cause
Be sure to check any medication you recently started.
Some antibiotics, anti-inflammatory pain relievers, acne medications, diuretics, and others can increase photosensitivity. Do not stop a medication on your own; it is safer to clearly tell the prescribing clinician or pharmacist that a rash appeared after sun exposure.
Reduce the use of perfumes and essential oils before daytime outings.
If only the areas where perfume was applied—such as the neck, wrists, or inner arms—become blotchy red or develop hyperpigmentation, a photocontact reaction may be suspected. Before outdoor summer activities, it is better to reduce strongly scented products.
Green tea or mung-bean-water baths are not standard treatments.
They may feel cooling as folk remedies, but when the skin is sensitive they may instead cause irritation. When symptoms are severe, prioritize cold-water compresses, moisturizing, and sun avoidance, and seek medical care if needed.
Signs That Dermatology Care Is Needed
In the following situations, do not rely only on self-care.
- Hives or a rash spread quickly after even a small amount of sunlight
- Blisters, oozing, bleeding, or peeling skin are severe
- The face, area around the eyes, or lips swell, or shortness of breath occurs
- Symptoms suddenly appear after starting a medication you are taking
- The rash lasts more than one week or recurs every year
- Fever, chills, severe pain, or whole-body symptoms occur together
Frequently Asked Questions
Q. Is sun allergy a real allergy?
A. Although it is commonly called sun allergy, it is actually a broad expression for several photosensitive skin diseases, including polymorphous light eruption, solar urticaria, and photoallergic or phototoxic reactions. Causes and treatment differ depending on the type.
Q. Is applying sunscreen well enough?
A. Sunscreen is important, but it is not a complete solution. Reducing outings during hours of strong sunlight, using physical barriers such as hats, long sleeves, and parasols, and checking causative medications and cosmetics are also necessary.
Q. What SPF should I use?
A. In general, a broad-spectrum product with SPF 30 or higher that blocks both UVA and UVB is recommended. People who spend a long time outdoors or are sensitive to sunlight should combine higher SPF with physical protection.
Q. Can I scratch when sun allergy develops?
A. Scratching can increase the risk of skin damage, hyperpigmentation, and secondary infection. Soothe the skin with cold compresses and moisturizer, and if itching is severe, receive treatment from a dermatologist.
Q. If I think it is caused by medication, should I stop the medication?
A. Do not stop it on your own. Tell the prescribing clinician or pharmacist that a rash appeared after sun exposure, and discuss whether an alternative medication or dosage adjustment is needed.
Conclusion
Sun allergy is one of the common skin discomforts experienced in summer, but its causes are more varied than many people expect. Unlike a sunburn caused simply by getting too much sun, it can involve recurrent itchy rashes after brief exposure or reactions related to medications, cosmetics, or perfumes.
The most realistic approach is not to avoid the sun completely, but to reduce and protect exposure in a way your skin can tolerate. Try combining sunscreen, long clothing, hats, parasols, cold compresses, moisturizing, and checking for causative ingredients. If symptoms recur or worsen, it is safer to see a dermatologist to identify the exact type.
This post may contain affiliate links. We may receive a commission from qualifying purchases.

